MEDICAL IMAGING SPECIALISTS

Mammography: The Evolution of Diagnostic Imaging
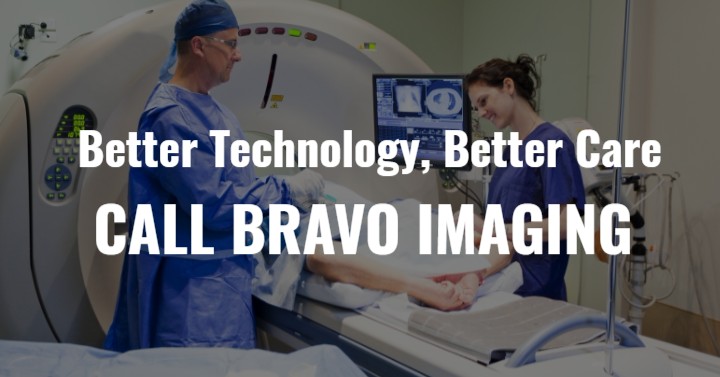
In the current practice of breast cancer detection and care, 3D mammography is the gold standard. However, 3D mammography was not used clinically until the early 2000s. Breast cancer has been heavily researched and been a public health concern since the early 1900s. With a span of over 100 years, you can imagine how the diagnostic technology has changed over the years. Here, we will explore the evolution of diagnostic imaging and how it has changed the practice of breast care.
Direct Exposure X-Ray
Prior to the 1930s, breast cancer was exclusively identified by palpation during breast exams. However, in the early 1920s, radiologists came to the consensus that early breast cancer or small tumor breast cancer could not be definitively diagnosed by palpation and inspection alone and radiographic imaging should be used to aid diagnosis. Early radiographic images of breast tissue were taken using the x-ray technology of the day which resulted in poor image quality and, because the breast tissue was not isolated, made it difficult to identify early or small tumors. In 1930, Stafford Warren, MD, standardized the use of x-ray technology to isolate breast tissue for a better breast mass diagnosis rating. Over the next few decades, mammography was honed as a radiology subspecialty and advances in how breast tissue was viewed emerged. The problem was that the new techniques used currently available devices and focused more on manipulating breast tissue to adapt to multi-purpose x-ray machines rather than modifying imaging modalities to view breasts specifically.
1970 Mammography
During the 1970s, John Wolfe, MD and Xerox worked together to develop a new breast imaging technique, Xeromammography, that was adapted from the xerographic photocopying process. The images were printed on paper rather than film, which made it more convenient for radiologists to read because it didn’t require special lights. However, a common problem was similar to that of regular xerox printing in that ink and toner could not be calibrated and had the potential of being misread because of nonuniform toner was high.
Over the rest of the 1970s, screen-film mammography technology offered the advantage of uniform-thickness tissue compression. Screen-film also added the advantage of faster processing times, increased contrast, and reduced radiation levels.
Emerging in the late 1970s, the oblique-view and two-view screening mammography allowed for even better tissue viewing and better diagnostics.
The New Age of Mammography
 Over the decades, technology continued to advance, and in the 1990s, mammography became more regulated, creating nationwide uniform standards for radiologists and breast cancer screening. In the early 2000s, digital mammography was introduced, eliminating film and wait times while improving the image quality. The added benefit of digital mammograms for patients is the decreased amount of radiation they are exposed to in the diagnosis phase.
Over the decades, technology continued to advance, and in the 1990s, mammography became more regulated, creating nationwide uniform standards for radiologists and breast cancer screening. In the early 2000s, digital mammography was introduced, eliminating film and wait times while improving the image quality. The added benefit of digital mammograms for patients is the decreased amount of radiation they are exposed to in the diagnosis phase.
Thermography was introduced as a new option based on the theory that cancerous tumors would exhibit higher temperatures than the surrounding tissue. However, it was proven to be insensitive to various tissues, and was discredited after lengthy trials.
Breast ultrasound has proven to be a useful tool in offering a definitive diagnosis for breast cancer. Ultrasounds are able to help determine the difference between solid and cystic breast masses and has led to an improved diagnosis. Ultrasounds allow for more specific diagnosis and have led to a decreased number of needless biopsies.
Breast magnetic resonance imaging (MRI) has evolved as a useful modality for diagnosis, presurgical planning, and ongoing evaluation of treatment success. Newer MRI machines have adapted to allow for comfortable isolation of breast tissue and contrast allows radiologists to accurately view curves and differentiate between tissue types. Typically, a breast MRI is done prior to mass treatment and then again after chemotherapy to assess changes and effectiveness of treatments.
Digital Breast Tomosynthesis (DBT) 3D Mammography
3D mammography uses layers to build images and allows radiologists to see through dense tissue to cancer underneath. Advances in tomosynthesis have provided a comfortable experience for patients in addition to superior imaging. The newest 3D mammography machines increase cancer detection by nearly 40 percent and decrease false positives by nearly 67 percent, which means better and more accurate patient care. DBT has been used to guide biopsies with improved outcomes and decreased insult to neighboring healthy tissue.
If your women’s clinic isn’t using the latest medical imaging technology for identifying and diagnosing breast masses, you should consider upgrading! For all of your ultrasound, MRI, and 3D mammography modality needs, contact Bravo Imaging. We buy, sell, trade, repair, install, and maintain the most up-to-date medical imaging equipment available on today’s market.
For more information on the history and evolution of mammography, check out these links:
https://pubs.rsna.org/doi/10.1148/radiol.14141233?url_ver=Z39.88-2003&rfr_id=ori%3Arid%3Acrossref.org&rfr_dat=cr_pub%3Dpubmed
https://pubs.rsna.org/doi/pdf/10.1148/radiographics.10.6.2259767
